
- Ingrown Toenails
- Bunions
- Corns
- Calluses
- Hammertoes
- Diabetic Foot Care
- Warts
- Heel Spurs/Plantar Fasciitis
- Athlete’s Foot
- Achilles Tendonitis
- Ankle Sprains
- Gout
- Heel Pain
- Toenail Fungus
- Blisters
- Ganglion Cyst
- Neuromas
- Plantar Fibroma
- RSD
- Sesamoiditis
- Ankle Injuries
- Rheumatoid Arthritis
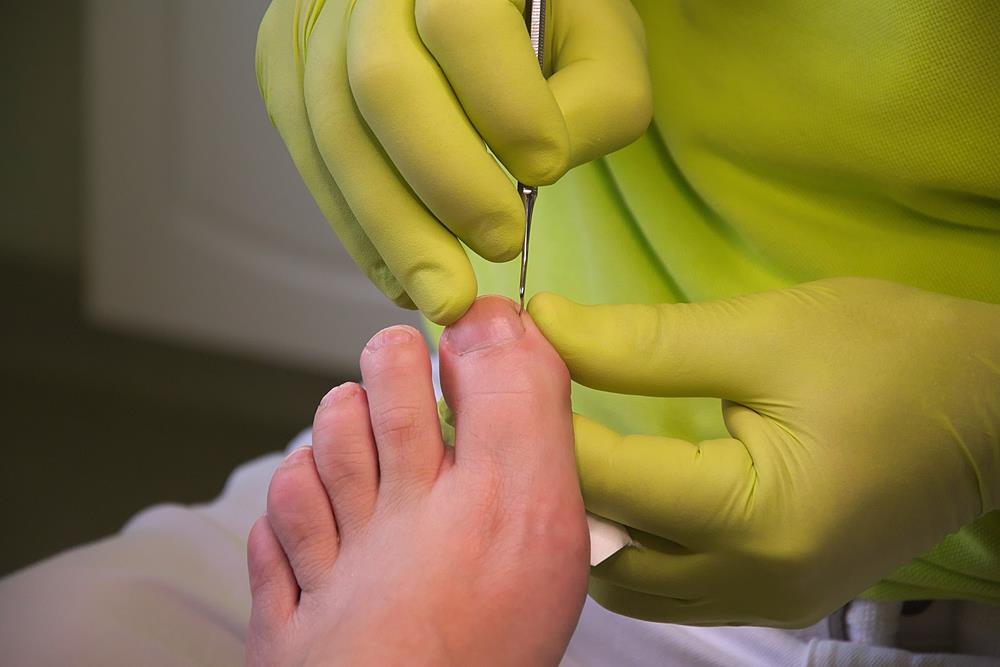
Ingrown Toenails
We have all made the painful mistake of trimming our nails too short at some point in our lives. Sometimes, this can really affect our foot health by causing ingrown toenails.
This happens when the nail grows downward into the skin instead of straight out, usually causing an infection. Ingrown toenails are most common on the sides of the big toe. It can also be caused by shoe pressure, injury, fungal infections, poor foot structure, etc.
Warm water soaks several times a day, properly fitted shoes and socks, and trimming nails in a straight line (rather than rounded) are ways to treat and prevent painful ingrown toenails. If there is an infection, seeing a podiatrist quickly is necessary to fix the problem. There are many different nail procedures that can be suggested for permanent relief from ingrown toenails.

Bunions
A bunion is a bony bump that forms on the joint at the base of your big toe. They can develop from an inherited structural defect, excess stress on your foot, or can result from an existing medical condition.
For the most part, bunions require no medical treatment. However, if you are experiencing pain, a podiatrist can help alleviate your symptoms.

Corns
Corns tend to be smaller than calluses and are the hard center is surrounded by irritated skin. While corns can be found on the bottom of the foot where pressure is usually applied, it is more common that you find corns on the tops and sides of your toes and even between your toes. When pressure is applied, corns can cause significant pain and discomfort.
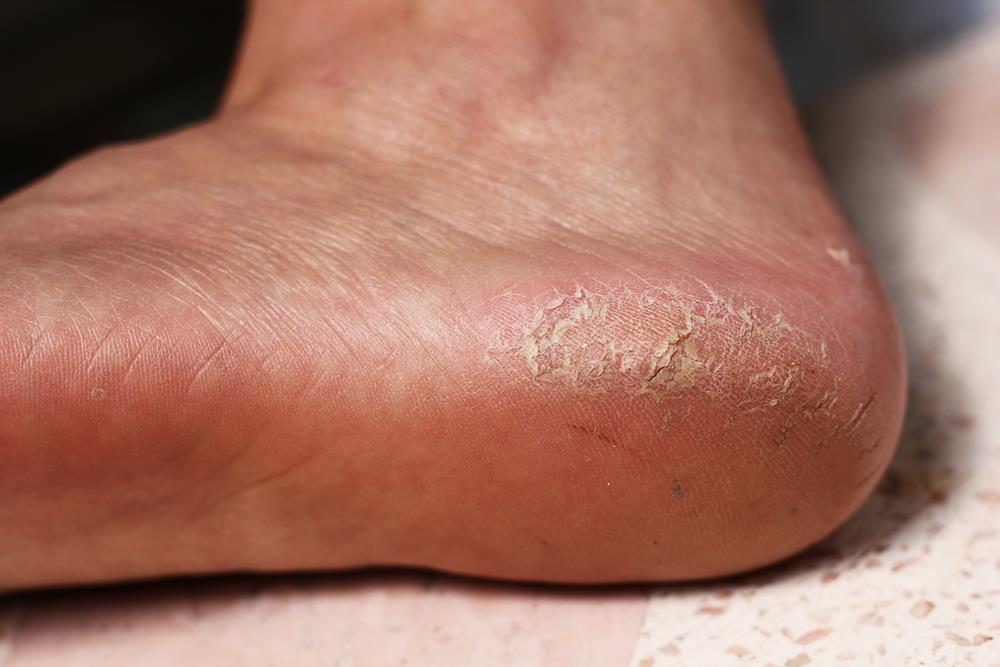
Calluses
Calluses, on the other hand, don’t usually cause pain. They usually develop on the soles of your feet, especially under the heels or balls, on your palms, or on your knees. Calluses vary in size and shape and are often larger than corns.

Hammertoes
Hammertoe is a deformity where one or both joints of the second, third, fourth or fifth toes begin to bend outside of their normal alignment. Pressure can begin to weigh heavy on the toes as you wear shoes which is where pain and other symptoms develop.
Hammertoes typically begin with small symptoms and deformities and continue to worsen with time. In its beginning stages, hammertoes are often impressionable which means they can be controlled using minimal treatment. It is important to know the signs of hammertoes to get them evaluated early. If left untreated, hammertoes can become more firm and difficult to manipulate, requiring surgery.

Diabetic Foot Care
Daily preventative care can help you decrease your risk of developing these other serious conditions like ulcers and infections. Inspecting your feet at the end of the day to look for any abnormalities, maintaining proper hygiene, keeping your feet warm in cold weather, encouraging blood flow in the feet, and maintaining an overall healthy lifestyle can discourage other conditions from developing.

Warts
Plantar warts are caused by the HPV virus and cause tiny cuts and breaks on the bottom of your feet.
While most plantar warts are not a major health concern, it is advised that you see a doctor to have the warts examined and treated. Some symptoms include small, rough lesions on the base of the foot, calluses in one spot, and tenderness when walking or standing for long periods of time.

Heel Spurs/Plantar Fasciitis
Plantar Fasciitis is a very common foot problem that can cause a lot of pain, and there are many different treatment options for plantar fasciitis. It is very important to see a podiatrist sooner rather than later after symptoms start to prevent long-term pain and to have the most success with treatment.

Athlete’s Foot
Athlete’s foot (tinea pedis) is a specific type of fungal infection that typically begins between the toes. A common cause of athlete’s foot is sweaty feet that are confined to tight shoes for a long period of time. Signs and symptoms of athlete’s foot include a scaly rash that usually causes itching, stinging and burning. Athlete’s foot is contagious and should be carefully monitored and treated. Athlete’s foot can easily be treated with antifungal medications, but the infection is likely to recur. Prescription medications also are available.

Achilles Tendonitis
Achilles tendinitis is caused by overuse of the band of tissues that connects the lower region of your calf muscle to your heel bone, also known as your Achilles tendon. Those at a higher risk for Achilles tendinitis are runners engaging in intense training or middle-aged people who participate in sports on occasion.

Ankle Sprains
A sprained ankle occurs when you twist your ankle in an abnormal way causing the ligaments holding your ankle bones together to stretch or tear. Most sprained ankles involve injuries to the ligaments on the outer side of the ankle. Treatment for a sprained ankle depends on the severity of the injury. Although you may just need proper rest and pain medications to heal, it is important to have the sprain looked at by a professional to determine the severity and proper treatment.
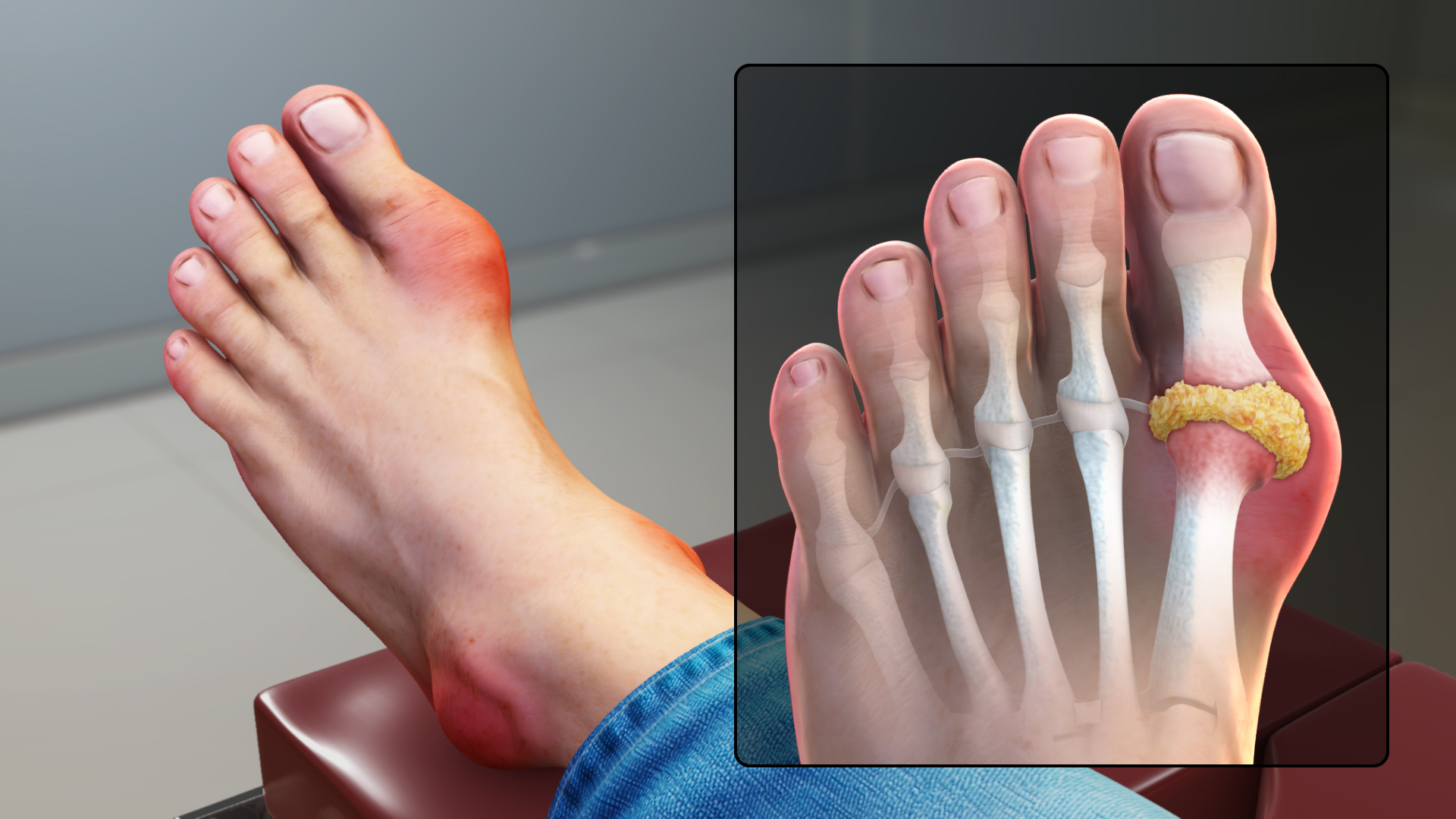
Gout
Often we associate arthritis with older patients who have lived an active lifestyle. Gout, on the other hand, can affect anyone. Gout is a common form of arthritis that is known for its sudden attacks of pain and joint tenderness. Joints that are affected by gout are often hot to the touch, swollen, and very tender. While symptoms are not chronic, it is essential to take preventative measures to manage gout as its side effects can be debilitating and intolerable.
- Stay hydrated. By drinking plenty of fluids and limiting sugary drinks, you can help prevent future gout attacks.
- Maintain a healthy weight as directed by your healthcare provider.
- Limit alcohol consumption. Some types of alcohol are more likely to increase the likelihood of a gout attack.
- Consider adding low-fat dairy products to your diet. These foods are proven to help protect against gout and are excellent sources of protein.

Heel Pain
Here at Foot and Ankle Center we offer services to help those patients who struggle with heel pain. Heel pain can be caused by a variety of conditions, and it is our goal to help determine and treat the cause of your pain rather than simply masking your symptoms.
Whether you are struggling with plantar fasciitis, a stress fracture, tendonitis, or even a cyst, we are here to help. Once your heel pain has a proper diagnosis, we can work with you to establish a customized care plan for your treatment.
For more information about our services or to schedule a consultation, contact us today at (423) 232-1771.
request an appointment
Toenail Fungus
If you routinely find your toenails yellowed and deformed, fungi may be to blame. There is a type of fungus that thrives in dark, moist, and warm areas, much like your shoes, shower, locker room, etc. You may notice yellow and/or white spots on the nail, along with a thickness that develops over time. If one nail is infected and left untreated, it can easily spread to other nails.
Treatments include a laser cleaning of the nail(s), oral medications, and medicated or non medicated anti-fungal cream.
Fungal nail infections require a process of treatments along with a continual effort to prevent it from recurring. Keeping the infection under control can include thoroughly washing and drying feet, applying anti-fungal cream, not sharing nail clippers or shoes/socks, wearing dry cotton socks and changing them often, wearing dry shoes, and using shower sandals in wet, public places.
For more information on how to treat fungal nail infections or to request an appointment, don’t hesitate to contact us today at (423) 232-1771! It’s important to nip the fungus in the bud before it spreads!

Neuromas
A neuroma can occur in many areas of the body when nerve tissue thickens. Morton’s neuroma is the most typical neuroma that occurs in the foot and it occurs between the third and fourth toes. Also known as an intermetatarsal neuroma, the name describes its location in the ball of the foot.
Compression and irritation typically cause the nerve tissue to thicken. This pressure creates inflammation of the nerve, ultimately causing untreatable damage to the nerves in the foot.

Ankle Injuries
Ankle injuries are one of the most common reasons for emergency room and doctors’ office visits. In fact, no fewer than 20% of all time-loss injuries in organized sports are ankle injuries. Ankle sprains and fractures may be difficult to distinguish since they share many of the same symptoms such as tenderness around the ankle ligaments and ankle bones. Localized swelling, discoloration and blister formation may be seen with more severe injuries.
Treatment
We initially treat ankle injuries with RICE: R est, I ce, C ompression, and E levation for a minimum of 24 to 72 hours. For more serious injuries, X-rays are critical to evaluate the integrity of the ankle. Significant swelling or deformity, accompanied by discoloration or numbness to the foot, may indicate a compromise to the nerves and circulation. This is a medical emergency requiring immediate attention. Merely putting an Ace wrap on a serious ankle injury is not sufficient. An under treated ankle injury may lead to years of pain and loss of function of the ankle joint.
The treatment of serious ankle injuries may require splints, casts or surgical intervention. The type of treatment varies based on the severity of the ankle injury. If surgical correction is inevitable, you want to make sure that you are evaluated by a specialist that mainly treats ankle injuries. An improperly treated ankle may lead to chronic pain and debilitation. After the initial treatment and stabilization of the ankle injury, orthotic devices are often used to help maintain the corrected or stabilized position, and to prevent re-injury.
Will I Need Surgery?
Serious ankle injuries may require surgical intervention. If an ankle is fractured or dis- placed, precise realignment is critical to avoid future problems such as arthritis of the ankle joint. Studies have shown that when the heel strikes the ground, five times the body weight is placed across the ankle joint. This pressure can be devastating to a poorly aligned ankle joint. A mere 1 mm displacement of the ankle bone reduces the ankle weight bearing surface by 42%. A slight misalignment can lead to severe arthritis and destruction of the ankle joint. The primary goal in the surgical treatment of a fractured or displaced ankle is realigning the joint surfaces and maintaining the length of the leg. We use the latest techniques in ankle surgery to get you back to your active lifestyle as quickly as possible. In fact, many times our patients are out of their cast and in physical therapy in as little as three weeks after surgical repair of their fractured ankle. This allows patients to resume their activities quickly and heal with fewer complications. Ankle arthroscopy is an innovative technique to evaluate and treat ankle injuries. It offers fewer complications and minimal soft tissue disruption while restoring function and stability to the ankle joint. Llaser ankle athroscopy is now used to resurface joint irregularities, remove binding scar tissue, and remove painfulbone spurs. This is an excellent treatment option available for either acute or chronic ankle conditions. When serious ligament injuries mandate an open repair, versus an arthroscopic one, the Brostrom-Gould procedure has been used to repair and stabilize acute or chronic ankle sprains. The procedure was designed to preserve the body’s natural anatomy, while repairing the ligaments. The advantage over traditional stabilizations is rapid healing with minimal, if any reduction, in the range of motion.

Rheumatoid Arthritis
Rheumatoid arthritis is a chronic inflammatory disease that causes the immune system to attack the joints. In some respects, this reaction is similar to an allergy, in which the body often reacts with a runny nose and itchy eyes. In rheumatoid arthritis, the autoimmune response can lead to permanent, painful changes in the joints.
The joints are the intersections of two bones. The ends of the bones are covered with cartilage (a smooth, durable substance) that allows bones to glide over each other with minimal friction. Cartilage also acts as a cushioning device to absorb forces. A structure called the joint capsule surrounds, stabilizes, and protects the joint. Within the capsule is a synovial membrane that contains synovial fluid (viscous substance similar to oil) that transports nutrients to the cartilage and keeps its surface well lubricated so the joints can work smoothly.
In rheumatoid arthritis, an autoimmune defect causes healthy cells to be attacked, releasing enzymes that attack surrounding tissues. One of these structures is the synovium in the joint. It becomes inflamed and causes swelling and pain.
Signs and Symptoms
Rheumatoid arthritis affects women three times more often than men. Typically, it affects the small joints first, including the joints of the hands and feet. More than one joint usually is affected, and symptoms often appear bilaterally. Symptoms are usually worse in the morning or after rest.
Subcutaneous rheumatoid nodules appear in about one-quarter of cases. Nodules are firm, pea-sized masses made up of inflammatory by-products and scar tissue. They are not painful and can occur anywhere in the body, most commonly in the elbow, the back of the forearms, the ankles, or the back of the skull.
Rheumatoid arthritis is a systemic disease. In addition to joint pain and stiffness, symptoms include muscle aches, anemia (low red blood cell count), and fever. These are very general symptoms, but if they occur repeatedly, they should not be overlooked.
Diagnosis
X-rays cannot confirm the presence of rheumatoid arthritis, but they are used to rule out other diseases. X-rays also establish a baseline for comparison as the disease progresses.
The latex test is used to diagnose rheumatoid arthritis. This test detects an antibody in the blood called the rheumatoid factor. Rheumatoid factor is present in the blood when the body reacts to inflammation in the synovial membranes. It is not always present at the beginning of the disease, but as the condition progresses, most patients with rheumatoid arthritis test positive for it. The rheumatoid factor is not exclusively a product of rheumatoid arthritis. It is an antibody produced in response to inflammation and other diseases that cause inflammation can also result in an elevated rheumatoid factor. These situations are rare, however, and the latex test can confirm a preliminary diagnosis of rheumatoid arthritis.
After the diagnosis is made, the physician determines if active inflammation is occurring in the body. This is done by a sedimentation rate test . In this test, blood is drawn and allowed to settle over a period of time. A high, or increasing sedimentation rate in the blood indicates active inflammation. A follow-up test determines if the inflammation is increasing or decreasing and the results determine if treatment is needed.
Treatment
Treatment for rheumatoid arthritis requires teamwork by the patient, the podiatrist, the general physician, and, most importantly, a rheumatologist . The medications and treatments for rheumatoid arthritis are constantly changing and a rheumatologist can provide the latest treatment options.
Initial treatment usually includes nonsteroidal antiinflammatory drugs, such Advil and Aleve, to reduce inflammation and pain. A drug called methotrexate can delay the progression of the disease.
Stretching exercises and corticosteroid injections also can reduce pain. Steroidal injections lose their effectiveness after three injections, however, after which their usage can become detrimental.